Before you read
This blog summarises a peer-reviewed article I wrote and published in the British Journal of Community Nursing (Chronic Oedema Supplement) in October 2023. The original paper presents a reflective case series examining women referred with complex arm swelling following breast cancer treatment. This page does not replace medical advice. Aromatase inhibitors are life-saving medications and remain central to breast cancer treatment. The purpose of this blog is to explain why some women develop swelling that does not behave as expected and to clarify what to do when standard management, including compression therapy, is not working.
A link to the full published article (PDF) is provided at the end of this page.
Why this article was written
Breast cancer-related lymphoedema is most commonly explained by cumulative lymphatic disruption following breast surgery, lymph node dissection/removal and radiotherapy. In clinical practice, however, this explanation does not account for all presentations. Some women develop arm swelling that does not follow expected lymphatic patterns. The swelling may appear months or years after surgery, is often painful or inflammatory, and does not respond as expected to standard lymphoedema management. In these situations, the cause is often unclear, particularly when compression therapy has been applied appropriately but symptoms persist or worsen.
This raised a specific clinical question: Could medication be contributing to these symptoms?
What led to closer investigation
Over a short period of time, several women were referred with painful arm swelling, most commonly affecting the forearm, hand or fingers. Across cases, the women were slim or of low-to-normal BMI, had completed surgery and radiotherapy without complication, and developed symptoms after starting aromatase inhibitor therapy. Importantly, the swelling did not behave like classical lymphoedema. It was reactive and inflammatory in nature, responded poorly to standard compression, and in some cases worsened rather than improved. The lack of response to compression was a key feature that led to further investigation.
What are Aromatase Inhibitors?
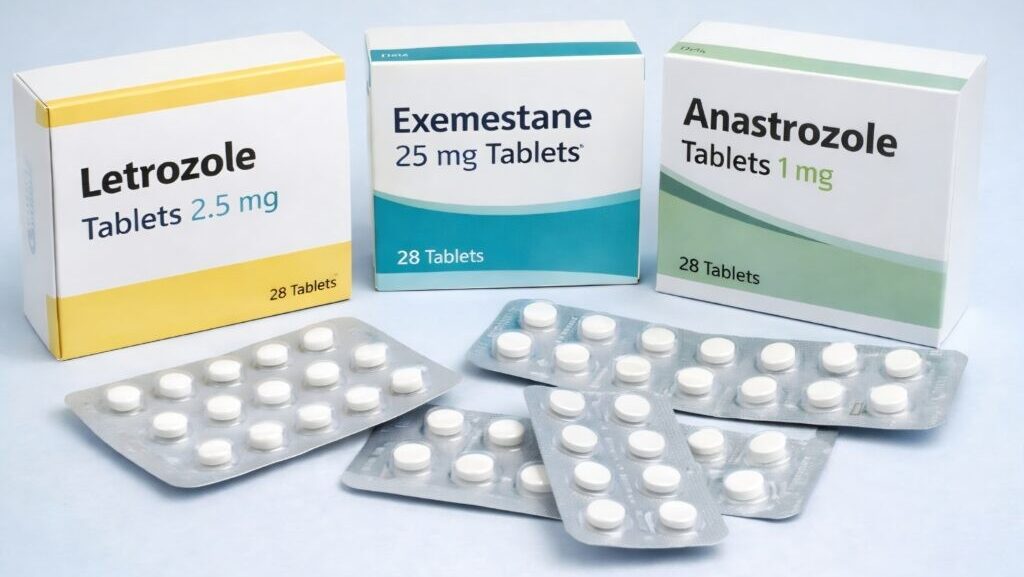
Aromatase inhibitors are prescribed after oestrogen-receptor positive breast cancer and reduce systemic oestrogen levels as part of long-term endocrine therapy. Commonly prescribed drugs include Letrozole, Exemestane and Anastrozole. This article does not challenge their role in cancer treatment. Instead, it examines whether endocrine therapy may contribute to specific tissue responses in a small number of women, particularly where swelling is inflammatory and non-responsive to compression.
Why slim women may be more affected
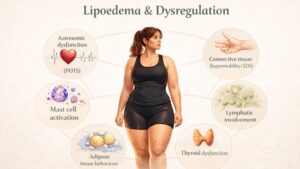
Adipose tissue contributes to background oestrogen production. Women with higher adipose mass retain some circulating oestrogen while taking aromatase inhibitors, whereas slim women do not. As a result, oestrogen reduction may be more abrupt, inflammatory signalling may be increased, and connective tissue reactivity may be heightened. In the case series, all women had a BMI below 25, with several being significantly lean.
Aromatase Inhibitor Musculo-Skeletal Syndrome (AIMSS)
Aromatase inhibitor therapy is associated with Aromatase Inhibitor Musculoskeletal Syndrome (AIMSS). Features include joint pain and stiffness, tendon pain, myofascial tightness and reduced hand function. In this case series, forearm and hand swelling appeared alongside these musculoskeletal features rather than occurring specifically as a lymphatic problem.
Axillary Web Syndrome
Several women had experienced axillary web syndrome earlier in their cancer treatment, before starting aromatase inhibitor therapy and symptoms persisted or evolved after endocrine therapy was introduced.This pattern suggests altered tissue behaviour and prolonged connective tissue reactivity rather than aromatase inhibitors being the primary cause of axillary web syndrome.
Reactions to Compression Garments
Compression is not neutral. In reactive or inflammatory tissue states, excessive or poorly matched compression can worsen symptoms rather than improve them. In these cases, cotton-ribbed, low-tension garments, often worn overnight, were better tolerated than standard circular-knit compression. This is particularly relevant where swelling does not improve with escalation of compression therapy.
Other Connective Tissue Symptoms
Alongside swelling, trigger finger, tendon pain, Dupuytren’s Contracture, reduced grip strength and difficulty with fine motor tasks were also observed. These findings point towards broader connective tissue involvement rather than isolated lymphatic dysfunction.
What the Cases Highlighted
The article describes five individual cases. Across these cases, there were consistent features, including non-responsive swelling affecting the forearm and hand, pain and tissue sensitivity and poor tolerance of conventional compression garments. In every case, women were referred back to their oncologist for a medication review. These findings do not suggest that aromatase inhibitors cause lymphoedema in everyone. They do suggest that, in some women, aromatase inhibitor therapy may act as a contributing factor when swelling is reactive, inflammatory and resistant to standard compression approaches.
What this means for patients
This article does not suggest stopping aromatase inhibitors or making changes independently. However, if a woman develops reactive oedema of the forearm or hand, particularly swelling that is painful, inflammatory or not responding to compression therapy, this should prompt further clinical review. In the cases described, each woman was referred back to her oncologist for a medication review to consider whether aromatase inhibitor therapy could be contributing to the tissue responses. The key message is that swelling which does not behave as expected should not simply be escalated with more compression, but assessed in the context of endocrine therapy.