Why I am concerned about the way compression is being discussed online
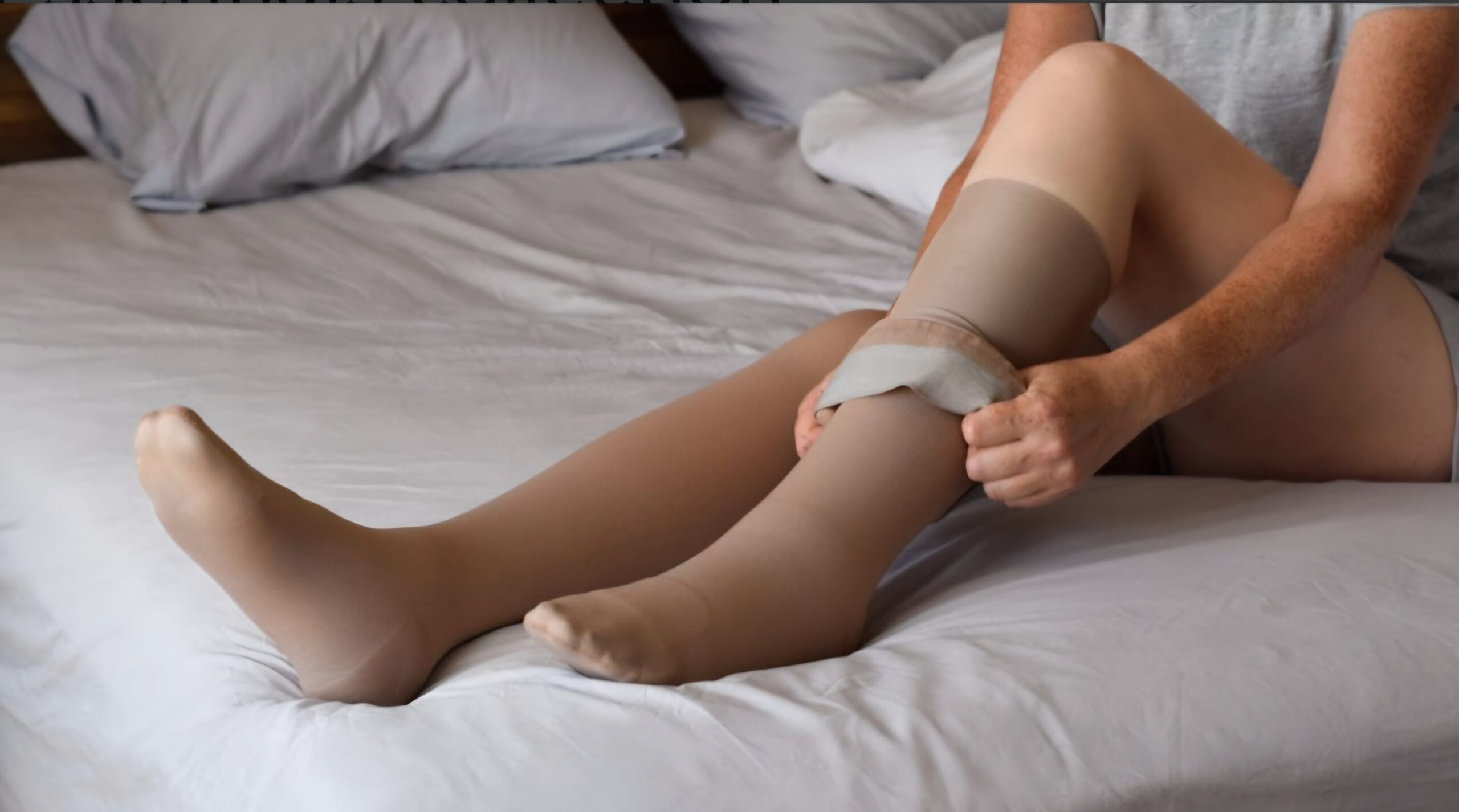
As a clinician working daily with people who have lymphoedema, lipoedema and chronic venous disease, I am increasingly concerned by the way compression garments are being discussed online. Compression is often presented as something you can simply buy, try and either believe in or dismiss, frequently based on experiences with fashion leggings, shapewear or so-called “lymphatic” garments sold online. Compression therapy is not a trend, a lifestyle product or a wellness accessory. It is a medical intervention. When it is used correctly, it can be genuinely life-changing. When it is misunderstood or misapplied, it can be ineffective at best and actively harmful at worst. This article explains what compression actually is, what it is not, why safety matters, and why so many people believe compression “doesn’t work” when, in reality, they have never experienced medical compression at all.
What compression is not
Compression does not work because something feels tight. Tightness is a sensation, not a treatment. Fashion leggings, sports “compression”, shapewear and recovery wear are not medical compression garments. They are not designed to deliver a measurable therapeutic dose, they are not engineered around limb shape, and they are not produced to clinical testing standards. Most non-medical garments apply uniform or random pressure rather than a planned gradient, are not manufactured to deliver a defined compression class measured in millimetres of mercury (mmHg), are not designed using the physical laws that govern how pressure behaves on limbs, and prioritise appearance, comfort and cost over mechanical performance. A garment can feel restrictive and still provide no meaningful therapeutic effect. Restriction and compression are not the same thing.
Compression is not automatically safe
One of the most concerning messages circulating online is the idea that compression is harmless and suitable for everyone. This is simply not true. Before compression is recommended, vascular and cardiac safety must be considered. Arterial disease is often silent and may be present without obvious symptoms. Early or undiagnosed heart failure may also exist, meaning the heart may not be able to tolerate the fluid redistribution and increased venous return created by compression. Applying compression to someone who is not safe to compress can reduce arterial blood flow, increase pain, worsen tissue ischaemia through reduced oxygen delivery, and delay wound healing, meaning compression can cause harm rather than benefit.
People who require proper assessment before compression include those with peripheral arterial disease, diabetes particularly when long-standing or poorly controlled, a history of smoking or significant vascular risk factors, cardiovascular disease, heart failure, previous vascular surgery or arterial stents, chronic kidney disease, advanced age with reduced arterial elasticity, peripheral neuropathy or reduced protective sensation, and non-healing wounds or ischaemic skin changes. Assessment comes before garments. If safety is not discussed, compression is being oversimplified.
“I’ve tried compression – it didn’t work for me”
This is something I hear frequently in clinic. When explored properly, it usually means one of two things. The first is that the person has only ever tried non-medical garments such as tight leggings, shapewear or “compression” bought online. If you have never worn medically graded, properly fitted compression, you have not actually tried compression treatment.
The second is that medical compression was used, but it was inappropriate — the wrong type, the wrong class or a poor fit. Compression that does not match limb shape, tissue characteristics or diagnosis can be uncomfortable and ineffective. That does not mean compression does not work; it means it was not correctly assessed or applied. This distinction matters because dismissing compression based on non-medical garments or poorly matched therapy can prevent people from accessing an intervention that, when used properly, can significantly improve symptoms, function and quality of life.
The physics that actually governs compression
Effective compression therapy is not based on intuition or how something feels. It is governed by physics. Compression is the controlled application of force over an area onto a living, deformable system, and its behaviour follows mechanical principles that are often ignored in marketing and online discussion. You do not need to memorise these laws, but they explain why professional assessment and fitting matter.
Laplace’s law: why compression must be graduated and directional
The most important physical principle underpinning compression garments is Laplace’s law, which describes the relationship between pressure, fabric tension and limb size. In simple terms, pressure equals tension divided by radius. This means smaller areas of the limb experience higher pressure, larger areas experience lower pressure, and the same garment delivers different pressures on different limb shapes. As a result, two people wearing the same compression class are not receiving the same physiological dose, and pressure also varies along the length of a single limb. For lymphatic transport to be supported, pressure must encourage movement from the extremities towards the root of the limb and central circulation. This requires a planned pressure gradient rather than uniform tightness. Graduated compression is therefore essential. Simply wearing a garment labelled with a compression class does not guarantee an effective or safe outcome. Compression is not a fixed property of a garment; it is the result of how that garment behaves on a specific body.
The law of cylinders: why limbs are not pipes
Compression is often described using plumbing metaphors such as “pushing fluid upwards”, but this is misleading. Fluid flow in rigid pipes follows very different rules from fluid movement in human limbs. Limbs are not rigid tubes. They are compliant structures that change shape during movement, contain multiple fluid compartments, and include valves, fascia and muscle activity. Compression does not create linear flow like water in a pipe. Instead, it alters pressure relationships within tissues and across blood and lymphatic vessels.
Starling forces (revised): compression as pressure rebalancing, not drainage
Modern understanding of capillary exchange recognises that fluid continuously filters out of capillaries and is returned via lymphatic pathways, rather than being reabsorbed venously in the way older models suggested. Compression does not mechanically drain fluid. By increasing interstitial pressure, it reduces excessive fluid leakage into tissues, limits ongoing swelling and supports lymphatic uptake where lymphatic function allows. Compression cannot overcome lymphatic obstruction and cannot replace active lymphatic pumping. Its role is pressure rebalancing, not forced drainage.
Movement, stiffness and working pressure
Compression garments are static devices applied to moving bodies, and their effects occur both at rest and during movement. At rest, compression helps limit further fluid accumulation. During movement, garment mechanics become crucial. Highly elastic, low-stiffness garments stretch easily and offer little resistance during muscle activity. They may feel snug, but they produce minimal pressure change during walking or muscle contra
ction. Therapeutic compression relies on appropriate stiffness. When a garment resists stretch, muscle movement creates pressure fluctuations that enhance venous return and support lymphatic efficiency. Movement does not make compression work; it amplifies what it already does. A garment that restricts movement, causes discomfort or is not worn consistently is not therapeutic. A garment that is not worn is not treatment. Different types of compression for lymphoedema, lipoedema and post-surgical recovery.
Compression is not constriction
A critical distinction rarely discussed online is the difference between compression and constriction. Non-medical garments often create local pressure points caused by tight cuffs, reinforced bands, seams or fabric rolling. These can worsen swelling below the area of pressure and reduce overall effectiveness. Therapeutic compression avoids turning the limb into a series of tourniquets and instead delivers a controlled, tolerable pressure profile that supports function rather than restricting it. Constriction is not compression. Tightness alone is not treatment.
Medical compression is prescribed, not discretionary
Medical compression is measured in millimetres of mercury, a unit of pressure used in the same way as blood pressure. It describes the therapeutic dose being delivered, not how tight something feels. Compression garments are selected based on diagnosis, limb shape and tissue characteristics, chosen in an appropriate compression class and knit type, professionally measured, fitted and reviewed over time. Compression is usually part of a broader management plan that may include manual lymphatic drainage, exercise, skin care and education. Compression alone is not a cure, but when used properly it is a powerful clinical tool.
My clinical position
Compression therapy remains one of the most valuable interventions we have for venous and lymphatic conditions, but only when it is applied with mechanical and physiological understanding. Not all compression is medical compression. Tight is not treatment. Safety is never optional. If you are considering compression, or feel it has not worked for you in the past, assessment matters. Measuring matters. Choosing the right garment matters. This is exactly what I do in clinic. If you would like compression to be assessed, prescribed and fitted by someone who understands the physics, the physiology and the risks, you are very welcome to get in touch — because compression works best when it is treated as what it really is: applied physics on a living system.